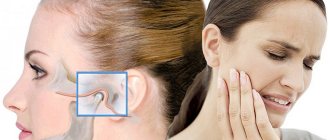
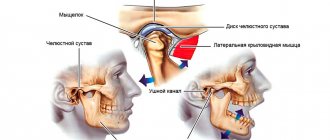
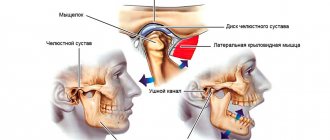
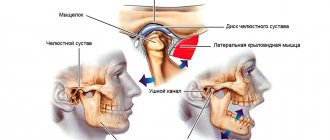
What is the temporomandibular joint - TMJ
We use this joint while talking, chewing, yawning, laughing - very often. Around it are muscles and tendons that allow the jaw to move in different directions for different purposes.
TMJ problems occur for many reasons:
- violation of the dental system, for example, congenital anomalies of teeth, gums or bone tissue, malocclusions, injuries, poor-quality prosthetics;
- congenital anatomical abnormalities of this joint;
- increased or decreased tone of muscle fibers around the TMJ;
- active conversational load, for example, among actors, singers, speakers;
- central nervous system problems;
- disruptions in the functioning of the endocrine system;
- excessive tension of the jaw muscles, for example, due to the bad habit of biting nails.
What is the temporomandibular joint and why do problems arise with it? Detailed and clear - in the video:
Actors and singers with active oratorical articulation are at risk for TMJ arthrosis
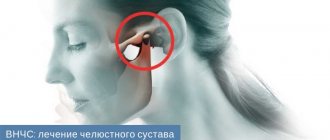
Pain in the temporomandibular joint
Temporomandibular joint dysfunction (TMJ) is one of the most common causes of facial pain and is often incorrectly referred to as temporomandibular dysfunction. There are 2 main types of TMJ dysfunction: myogenic (the source of muscle pain) and arthrogenic (the source of pain is the TMJ). Understanding TMJ Dysfunction
This disorder involves the presence of the following symptoms: - pain or discomfort in or around the ear, TMJ and/or muscles of the jaw, face, temple area and neck on one or both sides.
Pain can occur unexpectedly and increase in frequency and intensity over months and years. Mouth opening with a click, crepitus, closing, restriction of opening or deviation of the lower jaw during movement, difficulty chewing, and headache are also associated with TMJ. Structure of the TMJ The
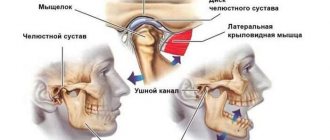
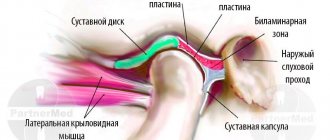
temporomandibular joint, or TMJ, is a freely rotating and sliding joint, covered with fibrocartilage, a football-shaped ball (condyle), a fibrous pad (disc), a bone socket for the pad (fossa), ligaments, tendons, blood vessels and nerves.
The disc functions as a moving shock absorber and stabilizer between the condyle and fossa. When the jaw opens, the condyle normally rotates first and then slides forward within the fossa with a disc located between the condyle and the fossa. Muscles of mastication
Muscles attached to the lower, upper jaw, skull and neck.
The muscles of mastication open, close, extend, and move your jaw, allowing you to speak, chew, and swallow. The accessory muscles of mastication (neck and shoulder muscles) stabilize the skull on the neck during chewing. Myogenic TMJ dysfunction (muscle-related)
Typically occurs due to overuse, fatigue, or tension in the masseter or accessory muscles, resulting in facial pain, headaches, and sometimes neck pain.
Arthrogenic TMJ dysfunction (joint-related)
Typically results from inflammation and degenerative changes in the hard and soft tissues of the joint.
Capsulitis or synovitis (inflammation), slipped disc (also called internal injury) and degenerative arthritis are the most common causes of TMJ dysfunction. Causes of TMJ Dysfunction The exact causes of TMJ
dysfunction are still unclear.
It is believed that the development of dysfunction is due to a combination of several severe factors, including injury and joint disease. Teeth clenching and grinding (bruxism), as well as tension in the neck and head muscles, are currently not proven causes of TMJ dysfunction, but they can aggravate the symptoms of this disease and must be taken into account in the treatment and management of patients with this pathology. It is important for patients with this dysfunction to understand that this disease can be chronic and can be very dependent on many factors, including emotional stability. Because there is no quick fix or emergency treatment for TMJ, the most successful and expert-supported treatments focus on self-monitoring and managing aggravating symptoms. Factors Associated with TMJ Dysfunction
- Trauma: Direct trauma to the jaw is associated with symptoms of dysfunction.
Direct trauma to the jaw can occur from a blow to the jaw, hyperextension (strain) of the jaw, and in some cases, compression of the jaw. Prolonged or forceful dental procedures, intubation during general anesthesia, and surgical procedures of the mouth, throat, and upper gastrointestinal tract (esophagus and stomach) can injure the TMJ. — Incorrect habits: Habits such as clenching teeth, clenching the jaw, grinding teeth (bruxism), biting lips or nails, chewing gum, and placing the jaw in abnormal positions are common. In relation to them, evidence of their involvement in the development of dysfunction has not been proven. Such habits are often associated with TMJ dysfunction and can contribute to the emergence of factors that translate into a chronic form and aggravate the existing symptoms of the pathology. — Occlusion: Dental occlusion refers to the way the teeth fit together or “bite.” Historically, dentists have viewed malocclusion as the primary cause of TMJ dysfunction. Recent studies have shown that malocclusion does not usually lead to this group of diseases, with the exception of a few cases. Each situation must be considered individually so that the doctor can make a differential diagnosis of facial pain. — Psychological factors: Many patients with TMJ dysfunction say that the onset of symptoms of the disease or worsening of its course is accompanied by an increase in emotional stress and psychological imbalance, leading to depression or anxiety. Scientific research shows that many patients with this dysfunction experience varying levels of depression and anxiety, and these levels are higher than those without this dysfunction. To date, it has not been established whether symptoms of depression or anxiety are present before the onset of TMJ dysfunction and then contribute to its formation, or whether chronic pain associated with this pathological condition leads to the formation of anxiety and depression. Many patients begin to clench and grind their teeth more frequently and intensely when they experience emotional stress, psychological imbalance, or pain. — Disorders of the temporomandibular joint: Some types of arthritis can lead to damage to the TMJ, as well as other joints. This is common in osteoarthritis developing in the aging population. Many other diseases, such as Parkinson's disease, myasthenia gravis, strokes, amyotrophic lateral sclerosis, can lead to excessive or uncontrolled movements of the masticatory muscles. — Other factors: Drug use and some prescribed medications can affect the central nervous system and muscles, and lead to TMJ dysfunction. Diagnosis of TMJ dysfunction.
Diagnosis of this disease should be part of routine practice among general practitioners and dentists.
A short set of diagnostic procedures may include: - History of the disease: complaints of pain in the jaw, headaches, neck pain, discomfort in the TMJ area, jaw closing, clenching of teeth, damage to the jaw, head, neck, as well as a history of cases of TMJ dysfunction or treatment of facial pain. - Objective examination: may include measurement of jaw opening, combined movements, jaw deviation during opening, palpation (finger pressure required) of the joint, jaw, head and neck muscles to determine pressure points and the presence of crepitus. It is also necessary to evaluate the gums, soft tissues of the mouth, teeth and make notes about the disease, the presence of dental lesions, as well as the symmetry of the jaw, face and head. If any abnormalities are found during the examination, a more detailed history should be collected and a more in-depth examination performed. Comprehensive assessment of TMJ dysfunction A comprehensive assessment may include:
- A complete analysis of all symptoms related to TMJ, head, neck, medical history, dental history, life history, heredity, psychological history.
— Comprehensive objective examination of the face, cervical spine, masticatory muscles, head and neck, neurological structures, teeth, gums, hard and soft tissues of the oral cavity. — Psychological history, including a short survey and testing. — Additional tests, including x-rays and imaging tests, biopsies, blood tests, urine tests, neurological tests, diagnostic injections. Treatment of TMJ dysfunction
Since there is no known cure for this pathology, the management of patients with symptoms of dysfunction is similar to the management of patients with other orthopedic or rheumatological disorders.
The goals of managing this group of patients are: reducing pain, adverse pressure and stress on the jaws, restoring jaw function, implementing a well-planned management program to treat the physical, emotional and psychological aspects. Management options and sequence of treatment for TMJ dysfunction are similar to other musculoskeletal diseases. As with many musculoskeletal disorders, the signs and symptoms of TMJ can be temporary and resolve on their own without developing serious long-term consequences. For these reasons, it is particularly important to try to avoid aggressive and irreversible treatment options such as surgery, major dental surgery or orthodontic treatment. Conservative management techniques include changes in behavioral habits, physical activity, medications, jaw exercises, and orthopedic devices. All of them have been found to be safe and effective treatments for cases of TMJ dysfunction. Most patients suffering from this disease achieve long-term remission with conservative therapy. Scientific studies show that in more than 50% of such patients, only a few symptoms persist or disappear completely. Self-monitoring of patients should include: - Limited jaw opening (no more than 2 fingers wide). — It is necessary to give your jaws a rest, avoiding prolonged chewing (chewing gum, bagels, tough meats). - Avoiding grinding and clenching of teeth by relaxing the jaw area and keeping the upper and lower rows of teeth at a distance. - Avoiding leaning or sleeping with the jaw resting. — Avoiding pushing movements with the tongue and chewing non-food items (nails, pens, pencils, etc.), stress, pressure on the jaw. - Use of cold, ice or moist-warm compresses, as prescribed by the attending physician or therapist. — Performing a massage of the affected muscles. - Perform gentle, limited jaw exercises as prescribed by your healthcare professional. — Use of medications as prescribed by the attending physician. Treatment options.
— Orthotics: You may be offered a brace (or a retainer known as a night watchman) that fits over your upper and lower rows of teeth.
The retainer has many different purposes, and it can be worn either constantly or part of the time, it all depends on the prescription of the attending physician. In most cases, retainers are used to separate rows of teeth, realign jaw joints, and help jaws relax. The unique style and adjustment of the brace will depend on your condition, how it changes while you wear the brace, and your overall treatment plan. Managing patients under stress.
One of the goals of treating TMJ dysfunction is to identify therapy for daily stress.
Your doctor may recommend several options for you to do this. These options include: biofeedback (biofeedback), breathing for relaxation, image management, and sometimes, referral to a specialist. Physiotherapy.
Physical therapists are specially trained professionals who assist in the rehabilitation of all types of physical injuries.
There are many treatment options that can help. These include: jaw exercises, posture training, ultrasound, electrical stimulation and mobilization. Your doctor and physical therapist will work together to formulate your treatment plan. Correcting your bite
Sometimes it is necessary to improve the way your teeth fit together.
This can be achieved in various ways. Orthodontics, usually with braces, will help move the teeth so they fit together better. In some cases, when the jaws themselves are not misaligned, they are corrected by a combination of treatment by an orthodontist and an oral surgeon. This is called orthognathic surgery. Correction of the bite occurs through the intensive work of the dentist, with the installation of crowns, bridges, and, if necessary, implants. This is done to replace missing teeth or to change the size and shape of teeth so that they fit together and function more harmoniously with the jaws and muscles. Surgery is sometimes performed to repair or reconstruct the jaws when conservative treatment fails to achieve comfort and good function. Surgery is rarely necessary, but it can be performed to remove debris that may have accumulated in the joint cavity, to repair damaged tissue, or even to replace the entire jaw, such as other joints (knees, hips, and shoulders). Conclusions
Extensive research is now being conducted to determine the safety and effectiveness of treatments for TMJ dysfunction/orofacial pain syndrome. Many researchers and clinicians advocate reversal and conservative treatment of dysfunction. Even when the symptoms of this dysfunction persist for a long time and are pronounced, many patients with this pathology do not require invasive treatment. Treatments designed to change the bite or reposition the jaws through orthodontic or dental reconstructive procedures are usually not necessary. And if they are used, then only when absolutely necessary. If permanent treatment is being considered for TMJ dysfunction or orofacial pain, we recommend seeking a second opinion. Specially trained dentists, physical therapists, psychologists and clinicians are often the best source of correct diagnosis and further management of this group of patients.
Exercises for the temporomandibular joint
How to understand what is bothering you with TMJ: 4 obvious signs
If you feel discomfort while talking, chewing, or yawning, look out for these signs:
- Are there any clicks or popping sounds during jaw operation (only 20% of people who notice this symptom complain of pain, however, this is a reason to suspect arthrosis of the temporomandibular joint and go for a diagnosis);
- Is there a feeling of jamming of the joint (if the fossa and the articular head are not in perfect contact, you have to open your mouth as much as possible, trying to find the right point);
- How severe is the pain (can occur when chewing, radiate to the temples, under the tongue, ears, neck, sternoclavicular region);
- Has your general health changed (headache and dizziness, insomnia, hearing impairment, depression and other uncharacteristic manifestations are possible).
With TMJ dysfunction, some patients develop snoring
How is arthritis of the lower jaw joint treated?
If pain and stiffness symptoms occur, it is necessary to ensure the TMJ rests. Move your jaw less, take only liquid food, and do not clench your teeth tightly. Visiting the dentist is a must. Only a qualified specialist will be able to tell why the joint is inflamed and prescribe the optimal treatment. Diagnosis consists of blood tests and x-rays. Depending on the situation, we recommend:
- cold compresses;
- drug treatment (broad-spectrum antibiotics, painkillers);
- physiotherapy.
If conservative treatment is ineffective, surgery will be prescribed. Traditional methods of treatment are not only ineffective for arthritis of the temporomandibular joint, they are often dangerous. Decoctions, compresses and ointments according to grandmother's recipes can relieve pain and swelling, but they will not remove the cause of the disease; moreover, some of them can inflame the joint even more. The consequences are impossible to predict, especially with the hematogenous method of infection of the joint. 20% of patients who treated themselves develop joint paralysis.
Treatment tactics
If there is no arthrosis, but there is dysfunction, the tactics are as follows:
- determine the root cause and eliminate it, for example, grind teeth and fillings that impede the functioning of the joint, correct prosthetic errors, and correct the bite;
- reduce the load on the joint - the patient is recommended to switch to soft foods, massage the facial muscles and exercises to relax the jaws;
- if the defects are serious, surgical treatment is performed - bone or muscle plastic surgery of the area of dysfunction.
If the doctor determines degenerative changes in the cartilage tissue, treatment for osteoarthritis will be prescribed. With the help of painkillers, they relieve pain. If necessary, a complex of physical therapy is prescribed, for example, laser or ultrasound. Good results are achieved by intra-articular injections of the Noltrex synovial fluid prosthesis, which restore the functionality of the joint by replenishing the missing lubrication.
Arthrosis of the TMJ is successfully treated with intra-articular injections of Noltrex
Factors that provoke the development of TMJ dysfunction:
Injury
Injury or overstrain of the jaw, or the habit of clenching the jaw tightly can injure the joint. Long-term dental procedures (or those in which the doctor uses force) and some other medical interventions can also lead to injury to the TMJ.
Wrong habits
Clenching teeth, clenching the jaw, grinding teeth (bruxism), biting lips or nails, chewing gum.
Malocclusion
At first, dentists generally considered this pathology as the main cause of TMJ dysfunction. But recent studies have shown that malocclusion, with rare exceptions, does not lead to such a disease.
Psychological factors
Many patients say that symptoms of TMJ dysfunction appeared (or worsened) due to stress, depression, or psychological trauma.
Temporomandibular joint diseases
Some types of arthritis can affect the TMJ (as well as other joints). For example, this sometimes happens with rheumatoid arthritis and systemic lupus erythematosus. Many other diseases (Parkinson's disease, myasthenia gravis, strokes, amyotrophic lateral sclerosis, etc.) can also lead to uncontrolled movements of the masticatory muscles.
What symptoms should you see a doctor for?
The earlier the diagnosis is made, the more favorable the prognosis. So seek help if:
- you experience pain in the lower jaw - intense or mild;
- you cannot fully move your jaw, you feel limited;
- hear a painful clicking or crunching sound when opening and closing your mouth;
- pain and noise in the ears appeared (especially if the otolaryngologist did not find any pathologies);
- There was a feeling of incomplete bite.
Arthrosis of the TMJ is not a very common phenomenon, but quite dangerous. Our usual comfort during conversation, eating, and other household activities is at risk. To avoid this, do not attribute alarming symptoms to fatigue and do not rely on “it will go away on its own”: be sure to find time for yourself and your health!
Dental pathologies
The temporomandibular joint hurts quite often due to problems with the gums or teeth. In such cases, discomfort may be reflected. Initially, they are localized in a certain area of the jaw, and then spread to neighboring areas of the face. TMJ pain sometimes occurs after installation of braces or removable dentures. Associated symptoms include recurrent headaches and excessive tooth mobility. Usually, after the correct bite is formed, all unpleasant sensations disappear without a trace. But if the pain persists for 6-8 weeks, you should contact your dentist for an examination. Also, discomfort in the TMJ area sometimes occurs several days or weeks after tooth extraction. The causes of acute or aching, pressing pain can be the following pathologies:
- alveolitis Post-traumatic infection and inflammation of the tooth socket. The pathological condition is characterized by severe pain, weakness, elevated body temperature, enlarged submandibular lymph nodes, and an unpleasant, putrid odor from the mouth;
Alveolitis.
- phlegmon. This is a purulent process without clear boundaries, caused by Staphylococcus aureus, prone to spreading to surrounding tissues. The upper and (or) lower jaw swells, when trying to open the mouth, acute pain occurs, there is a lack of appetite, hyperthermia, facial asymmetry, weakness, drowsiness, apathy;
Phlegmon of the lower jaw.
- abscess of the jaw area. In the connective tissue structures, a cavity is formed, limited from the surrounding tissues and filled with purulent contents. An abscess is characterized by swelling, elevated body temperature, skin soreness, fluctuation, headaches, hyperemia, malaise, and sleep disturbance.
Abscess.
But the most dangerous pathology is osteomyelitis, which affects the temporomandibular joints. With the development of a purulent infectious-inflammatory process, all structural components of the jaw bone are gradually involved in it. In the absence of medical care, osteonecrosis occurs. Clinical manifestations of osteomyelitis of the jaw include weakness, fever, chills, pain, limited mouth opening, tooth mobility, inflammatory infiltration of the soft tissues of the face.
If your temporomandibular joint hurts, it is advisable to first consult a dentist. The doctor will conduct the instrumental and laboratory tests necessary to make a diagnosis. The dentist will eliminate pathologies that correspond to his profile, or refer the patient to other specialists for further treatment.
Clicking in the jaw
Sometimes it happens that when you open your mouth or chew, your jaw clicks. Many of those to whom this happens usually do not pay attention to the clicks. For the time being, until other more unpleasant symptoms appear.
Click mechanism
Actually, the click itself occurs when the articular surfaces in the temporomandibular joint slip. As you can guess from the name of this joint, it is formed by the head of the lower jaw and the temporal bone and is located in front of the ear. Normally, when chewing or opening the mouth, the articular surfaces slide smoothly relative to each other and no clicking occurs. Moreover, both the left and right joints should move symmetrically. When even a slight asymmetry in movement occurs, both joints are affected at once.
If dysfunction of the temporomandibular joint develops (disturbance in the relationship within the joint, ligaments and muscles), then smooth movement in the joint is not possible. The head moves incorrectly and does not immediately snap into place, causing a clicking sound.
Dysfunction often precedes arthrosis (damage to articular surfaces). With dysfunction, the joint itself may still be intact, but due to asymmetry, the surrounding muscles and ligaments are overstrained. The cause of dysfunction and subsequent arthrosis can be trauma to the jaw, as well as structural features of the jaw (for example, malocclusion), as well as improperly installed dentures and fillings.