Causes of childhood stomatitis
There are 6 main factors that can provoke the occurrence of stomatitis in the mouth in infants:
- infections;
- mechanical damage;
- physical agents;
- chemical burns;
- allergic reactions;
- poor oral hygiene.
All conditions that cause immunodeficiency in a child predispose to the occurrence of such a pathology: chronic diseases of internal organs, vitamin deficiencies, the presence of foci of chronic infection in the body, stress, climate change. Dr. Komarovsky notes an increase in the incidence of stomatitis in children who often suffer from ARVI.
Infectious forms of the disease are the most widespread. Most often, herpetic stomatitis occurs. Also, lesions of the mucous membranes of the oral cavity can appear against the background of various infections: smallpox, measles, rubella, entero- and adenoviruses. Banal staphylococci and streptococci, which normally live in small quantities in the mouth of every baby, also play a huge role in the development of the inflammatory process. Their effect increases only when the child’s immunological status decreases.
Quite often, after taking antibiotics (especially if the course of treatment is long), infants develop a fungal infection of the oral mucosa - candidiasis or thrush, which can also trigger the development of stomatitis.
Children, especially young children, learn about the world around them through taste. Therefore, babies constantly put into their mouths all the objects that are at their disposal. Thus, mechanical trauma to the mucous membranes simply cannot be avoided. And take into account the fact that objects are not always clean, inflammation forms very quickly. A child can independently injure the mucous membrane by biting it with his teeth. This is observed very often in dreams with neuroses.
When teething, gums are sometimes injured, which, coupled with the baby’s reduced immunity during this period, leads to a strong inflammatory response.
Of the physical agents, the most common cause of stomatitis is exposure to hot food. In this case, microburns occur on the mucous membranes, at the site of which inflammatory foci are formed.
Chemical burns occur due to accidental exposure of the oral mucosa to potent substances. In everyday life, this could be vinegar, high-concentration hydrogen peroxide, alcohol or eau de toilette, perfume, various paint solvents or liquid cleaning products.
Anything can act as an allergic component in the development of stomatitis. For example, harmless candy, toothpaste, chewing gum, various drinks, medications and food. Often, allergic stomatitis occurs in infants during the period of introducing the first complementary foods.
Treatment with folk remedies
Alternative treatment can be a good addition to the main therapeutic prescriptions. However, only a doctor should decide how and how much stomatitis is treated in a child.
Traditional methods are not recommended for very young children. It is better not to use them before the age of 2 in order to avoid the development of serious allergic reactions, which can only aggravate the underlying disease.
Often, beekeeping products are used in folk recipes for medicinal purposes for stomatitis: honey and propolis.
- Dissolve 2 teaspoons of natural honey in the prepared decoction of chamomile flowers (1 tablespoon per glass of boiling water). Rinse your mouth with a warm solution 3-4 times a day.
- Mix a tablespoon of fresh aloe leaves with the same amount of natural honey. Apply the resulting mixture 3 times a day to areas of inflammation using a sterile cotton swab.
- Dissolve 10 drops of propolis alcohol tincture in a full glass of warm boiled water and rinse your mouth thoroughly 3 times a day after meals.
Gargling with soda and salt has proven to be a good remedy for treating stomatitis, even in young children. To prepare the solution, you need to dissolve half a teaspoon of baking soda and salt in a glass of boiled and cooled water. Rinse your mouth 4-5 times a day, especially after eating. However, it should be remembered that it is not advisable for the soda-saline solution to come into contact with open wounds on the mucous membrane.
Traditional medicine often prescribes treating stomatitis in children with burnt alum, a powder prepared from heat-treated potassium alum. To prepare the remedy, half a teaspoon of powder is dissolved in a glass of warm water until a somewhat viscous solution is obtained. Older children can rinse their mouth with this product 3-4 times a day. For babies, you can treat the mucous membranes with a swab dipped in alum solution.
Treatment of inflammatory diseases of the oral cavity with herbs has proven itself well. For this purpose, decoctions of sage, calendula, chamomile, and oak bark are used. They have a pronounced antiseptic and astringent effect. It is recommended to rinse your mouth with such herbal decoctions at least 3-4 times a day.
Symptoms and signs
How to recognize stomatitis in children? Despite the abundance of causes that cause this disease, all forms of stomatitis have common clinical symptoms:
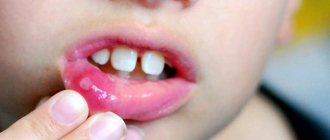
- The first signs of such a pathology are slight redness on the mucous membranes, which can be localized both on the gums and on the palate, on the tongue or on the lip.
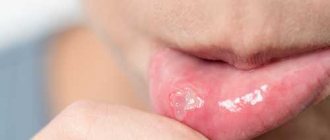
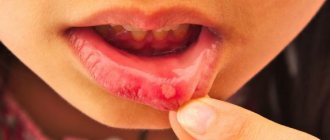
- Gradually, the redness gives way to swelling, round or oval ulcers appear, covered with a whitish or gray coating on top and surrounded by a red cushion. These ulcers are very painful and prevent the child from leading a normal life, eating or sleeping.
- As the inflammatory process becomes more severe, small ulcers merge into one large one.
- Local signs of stomatitis are accompanied by general symptoms: the child’s temperature rises, weakness, and lack of appetite appear.
One of the features of the course of the disease is the appearance of vomiting with stomatitis. It is caused by increased work of the salivary glands and increased excitability of the baby’s nervous system due to severe pain.
How to treat stomatitis in children at home?
On the Internet you can find descriptions of many ways to treat stomatitis in children at home. However, experts consider many of these virtual tips not only useless, but also dangerous. There is always a risk of allergies, so you should not use infusions and decoctions, even if you are absolutely sure that it will not harm the child. Instead of wasting time, it is necessary to undergo diagnostics and consultation with a dentist and pediatrician, who will prescribe the correct treatment regimen.
Types of childhood stomatitis and their main manifestations
The classification of childhood stomatitis is based both on the cause of the disease and on some distinctive features in the clinical course of such pathology. We will tell you how to determine this or that type of disease in our article later.
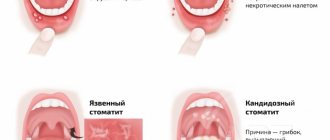
Catarrhal stomatitis
It is the mildest and most common form of the disease. In this case, multiple inflammatory foci appear on the mucous membrane of the gums, cheeks or lips, covered with a whitish coating, but without the formation of aphthae or ulcers. In this case, the child will complain of pain in the mouth when eating, drinking or talking, increased salivation, bad breath, and general weakness.
With catarrhal stomatitis, the mucous membrane is very susceptible to injury and bleeding, even during normal activities: brushing teeth, eating. When inflammatory foci are localized only on the gums, the clinical picture of stomatitis will resemble gingivitis.
Ulcerative stomatitis
The ulcerative form is a consequence of untreated catarrhal stomatitis. In this case, against the background of edematous foci of redness, multiple ulcerations are formed, which gradually increase in size, spread deep into the tissue of the mucous membranes or merge with each other.
The child complains of severe pain in the oral cavity, which intensifies when trying to brush his teeth or eat, and the smell of his breath becomes putrid. General health worsens: body temperature rises, weakness and body aches occur.
Young children are capricious, refuse to eat, and have trouble sleeping.
Gangrenous stomatitis
The gangrenous form of the disease is a continuation of catarrhal and ulcerative forms. A characteristic sign of this pathology is the spread of the inflammatory process deep into the tissues of the jaw with the development of extensive necrosis, which can involve the bones and spread to other anatomical areas.
The condition of a child with gangrenous stomatitis is extremely serious. There may be disturbances of consciousness, severe weakness, and the smell of rotting meat from the mouth. Regional lymph nodes are enlarged and painful on palpation.
Candidiasis (fungal or milk) stomatitis
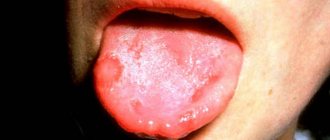
Candidal stomatitis is characterized by specific symptoms. At the onset of the disease, children have dry mouth. Subsequently, a burning sensation and an unpleasant aftertaste appear. A white coating in the form of small dots is deposited on the mucous membrane. As the process progresses, the points merge into a large lesion that resembles a curdled mass. Such plaque is difficult to remove, exposing the inflamed surface of the mucous membrane.
Fungal stomatitis often occurs without fever, and the general condition is little affected.
Infectious stomatitis
The phenomenon of stomatitis can also be observed in some infectious diseases. With scarlet fever, the typical picture on the mucous membranes of the mouth will be supplemented by specific manifestations of the disease: a pinpoint rash on the skin and a “crimson tongue” - the surface of the tongue is bright red, shiny with hypertrophied papillae.
With diphtheria, damage to the gums will be combined with the detection of dense grayish films on the tonsils or in the throat. In this case, a paroxysmal cough with episodes of suffocation will be noted.
Allergic stomatitis
The allergic form of stomatitis most often affects children over 4 years of age. It is characterized by a clear connection with the action of the allergen, a rapid increase in symptoms and their rapid extinction with adequate treatment. The clinical picture in this case is similar to the ulcerative version of the disease - ulcers or aphthae form on the mucous membranes, covered with a whitish coating and surrounded by a focus of redness. Quite often, this pathology occurs in the form of chronic stomatitis with periodic episodes of exacerbation.
Traumatic stomatitis
In cases of mechanical trauma, a significant focus of infiltration appears on the mucous membrane, which ulcerates as the inflammation progresses. When burned by hot drinks, a bubble often appears, after opening which a fairly deep ulcer is exposed. A distinctive feature of the traumatic form of the disease is a clear connection with trauma or thermal burn of the oral mucosa and the formation of a single lesion.
In case of severe inflammation, local symptoms may be accompanied by general symptoms: fever, malaise, headache.
Herpetic stomatitis
In herpetic stomatitis, the main morphological element is small blisters located against the background of a hyperemic mucous membrane. They quickly open and erosions form, which are covered with fibrous plaque. The lesions can be localized separately or merge into a single affected area.
Erosion is extremely painful, the child refuses to eat, is capricious, sleep is disturbed, and in severe cases there is a significant increase in body temperature. In this case, typical herpetic lesions can be found not only in the oral cavity, but also on the face or other parts of the body.
Bacterial (purulent) stomatitis
Most often, bacterial stomatitis appears due to constant improper oral care or microbial sore throat. The clinical picture is typical for stomatitis: initially foci of inflammation appear, which then transform into deep ulcers covered with abundant purulent plaque.
At the same time, purulent deposits on the tonsils are detected, the child’s general well-being suffers, body temperature often rises significantly, and the cervical, submandibular and clavicular groups of lymph nodes enlarge.
Vesicular stomatitis
Vesicular stomatitis is an infectious disease. Its causative agent is vesiculovirus, a virus transmitted from sick animals to people. The incubation period of this disease is 5-6 days, during which children may complain of fatigue, weakness, and slight chills. Subsequently, small painful blisters with whitish contents appear on the mucous membranes of the oral cavity. Similar elements appear in the area of the feet and hands.
The general symptoms are very similar to a banal acute respiratory infection: the body temperature rises, there may be signs of rhinitis and conjunctivitis. If the intestines are damaged, there may be dyspeptic symptoms: diarrhea or constipation.
Traumatic stomatitis
Inflammation of the mucous membrane in the mouth can be preceded by trauma: mechanical, thermal, chemical, radiation1,6.
Small children who put everything in their mouths can injure the mucous membranes with the sharp edges of toys or household items. Injuries often occur due to inept use of cutlery as a result of falls. In older children, stomatitis may be associated with a thermal burn, blows to the teeth, or the bad habit of chewing a pencil or pen. Sometimes the cause of inflammation is dental diseases and their treatment: sharp edges of damaged teeth and fillings, braces and aligners1.
When stomatitis develops in a child on the gum, on the inner surface of the cheek or in another place, the mucous membrane becomes red and swollen, and a painful erosion or ulcer may appear in the area of damage. Since there are many microorganisms in the mouth, there is always a risk of a bacterial or fungal infection1.
If the mucous membrane is constantly injured, painless whitish or whitish-gray layers may form on it.
In children under 1 year of age, stomatitis can be the result of using the wrong nipples: long, tight, irregularly shaped. The resulting Bednar aphthae are located in the area of the transition of the soft palate to the hard palate and are round erosions or ulcers1.
Treatment of traumatic stomatitis in children includes:
- elimination of traumatic factors;
- rinsing the mouth, irrigating the mucous membranes and treating wounds with drugs with an analgesic and antiseptic effect1.
Up to contents
Nutritional Features
Due to the fact that painful ulcers appear in the mouth with stomatitis, any meal gives the baby discomfort. Therefore, the diet during the period before recovery should have a number of features.
- All food taken should be warm and at a temperature as close as possible to body temperature. This will prevent unnecessary irritation and will not cause acute pain.
- Since chewing is quite painful, portions should be reduced by about a third, but the frequency of meals should be increased.
- When feeding your baby, you should give preference to dishes with a soft consistency, and it is better to postpone dense and dry foods until complete recovery.
- It is worth giving preference to products with a neutral taste. These are potatoes, bananas, pears, pumpkin.
- Until recovery, spicy, salty and sour foods are completely excluded from the child’s diet.
- To make eating less painful, you can purchase thick straws for cocktails and crush all food so that it can be drunk.
- The emphasis is on healthy foods rich in microelements and vitamins. For example, buckwheat, oatmeal, and rice can be recommended for cereals. It is preferable to give your baby cauliflower and broccoli as vegetables.
Caring for a child with stomatitis
The participation of parents in treatment and proper care of the child is not just important - they are decisive. With stomatitis, it is necessary to strictly follow the treatment plan, which is often very labor-intensive, so the result depends on parental care and control. The oral cavity is a kind of epicenter of pain, so it is not surprising that the child will be capricious a lot. Therefore, it is important for parents to be patient and persistent.
Nutritional Features
Most mothers and fathers are concerned about the question of how to feed a child with stomatitis. Firstly, it is necessary to eat only soft, warm and mushy foods, for example, in the form of purees. The main thing is that the food is high in calories and not heavy, because the child’s immunity is already weakened. After eating, be sure to rinse your mouth so as not to provoke the development of stomatitis and not to add any additional infection. If a child is ill, the diet should include the exclusion of spicy, sour, sweet foods and citrus fruits.
Pain relief and care
For stomatitis in children, pain relief is necessary. It is carried out with the help of various medications in order to avoid food refusal and poor sleep. In addition, for stomatitis in children, proper treatment of the oral cavity is very important. A doctor should recommend what to treat and rinse a child’s mouth with.
Is stomatitis contagious?
Infectious variants of the disease are quite easily transmitted from sick children to healthy ones. Most often, the infection spreads through airborne droplets from saliva during normal talking, coughing or sneezing.
The herpes virus can pass from an infected mother to the child during childbirth or during breastfeeding in the event of an exacerbation of herpetic inflammation.
We must remember that some forms of infectious stomatitis may well be transmitted through shared objects. This is especially true for cutlery, toys and personal care products. Therefore, if a child gets stomatitis, it is necessary to take measures aimed at preventing the possibility of its transmission to healthy children.
- If there is another child in the family, then it is worth protecting him from communication with the sick baby for at least a few days.
- It is imperative to provide the patient with individual household items that can be processed separately from the belongings of the rest of the family.
- If a case of stomatitis is detected in a kindergarten, it is recommended to disinfect all toys that healthy children may come into contact with.
Chronic aphthous stomatitis
Causes
Aphthous stomatitis is caused by staphylococcus, a microorganism that is found in large quantities in dental plaque and lives in carious cavities. Every person has this microbe and usually does not manifest itself in any way, but against the background of immune disorders. Often aphthous stomatitis can develop against the background of allergies, gastrointestinal diseases or injuries to the oral mucosa. Another factor in the development of the disease is dirty hands. This disease is often associated with children putting unwashed toys into their mouths, thereby increasing the total number and variety of microbes in the mouth.
Symptoms
Most often, manifestations of chronic aphthous stomatitis occur on the lips, transitional fold, gums, under the tongue and on the tongue - in places where the mucous membrane can be injured by teeth or spicy food.
- Minor change in general health. Characterized by enlargement of the submandibular lymph nodes, fever and weakness.
- On an externally unchanged mucosa, aphtha appears - a spot 5-10 mm in size, slightly rising above the surface of the mucosa, covered with a whitish film tightly fused to the mucosa and surrounded by a bright red rim. Aphthae are very painful when touched. Most often there are one or two aphthae, less often – several.
Must remember! It is necessary to accurately determine the type of stomatitis: herpetic or aphthous. With herpetic stomatitis, there are many small blisters that turn into erosions and sometimes merge with each other, and rashes on the lips are possible. With aphthous rashes, larger, single rashes occur only in the mouth. If you have stomatitis, you should definitely consult a dentist to determine the type of stomatitis and choose the right treatment tactics.
Treatment
Elimination of the factor that caused the disease:
- exclude all allergens (citrus fruits, chocolate, brightly colored foods...);
- if you are taking medications that can cause allergies, then you also need to take this into account (tell your doctor what you are taking and for how long);
- exclude rough, spicy, salty, sour foods;
- if stomatitis is caused by allergies, antihistamines (suprastin, loratadine) are prescribed;
- If the aphthae is due to injuries from sharp edges of a tooth or filling, it is necessary to put the tooth in order.
- in the first 3-4 days, treatment of aphthae is carried out exclusively with antiseptics (rinses, gels). You can use chlorhexidine, rotokan, miramistin, givalex, stomatidine, listerine, chamomile and calendula decoctions - you can take any of these drugs (or any other analogue). Use according to the instructions (there are preparations in ready-made form, and there are those that need to be diluted). Rinse (or wipe the mucous membrane in small children) 3-4 times a day.
- after 3-4 days, epithelializing agents are added: solutions of vitamins A and E, rosehip or sea buckthorn oil, solcoseryl.
- If relapses occur frequently, you should pay attention to your general health. In some cases, only joint treatment with an immunologist, gastroenterologist, endocrinologist and other specialized specialists can help cope with the disease.
Must remember! Aphthous stomatitis is, first of all, a microbial lesion. Oral hygiene, adherence to personal hygiene rules, as well as timely treatment of caries, caries complications, and removal of tartar in many cases are sufficient to avoid aphthous stomatitis.
How many days do people suffer from stomatitis and what to do at the first signs of it?
How long does stomatitis last? This question is of great concern to parents of sick children, since all the symptoms of the disease are unpleasant and cause discomfort to the child.
The duration of the disease depends on its form. Acute variants of stomatitis with adequate drug treatment resolve within 14 days.
If the disease does not go away for a month or more, then they talk about the chronic course of such a pathology. In this case, it is possible to alternate periods of subsidence of clinical symptoms and their exacerbation - recurrent stomatitis.
If you suspect signs of stomatitis in your child, you should urgently consult a doctor who will tell you how to numb the mucous membrane and prescribe comprehensive treatment. If it is not possible to visit a doctor as soon as the first symptoms of the disease begin, then it is possible to independently numb the mouth with local drugs (Dentinox, Kalgel). And you can’t delay medical consultation!
Viral stomatitis
About 80% of all stomatitis in children is caused by herpes viruses3,5. In approximately 70% of cases, the disease develops in children aged 1 to 3 years3,4.
The disease can occur in mild, moderate and severe forms.
With mild herpetic stomatitis, the general condition is practically not disturbed. Body temperature does not exceed 37-37.50 C. Symptoms of inflammation are limited to swelling of the gums and usually the simultaneous appearance of single painful herpetic blisters and erosions on the mucous membrane (no more than 6). After 1-2 days, the contours of the lesions are blurred, the rashes turn pale, and the erosions heal without scarring3.
With moderate stomatitis, the child’s temperature reaches 38-390 C and lasts until rashes continue to appear. General intoxication manifests itself in the form of weakness, headache, nausea. The child becomes capricious, lethargic, refuses to eat and play3.
As the temperature rises, the oral mucosa becomes red and swollen, and the gums begin to bleed. The number of herpetic elements reaches 20-25, repeated rashes are accompanied by fever3.
Severe stomatitis in children looks like a common acute infectious disease and is accompanied by severe intoxication: fever 39-400 C, chills, headache, aching muscles and joints, heart rhythm disturbances, nosebleeds, nausea and vomiting. The number of herpetic elements can reach 100; they are located not only in the mouth, but also on the skin of the face, on the eyelids and conjunctiva of the eyes, and earlobes. In addition, upper respiratory tract symptoms may be present.3
Treatment includes treating the affected area with painkillers and antiseptic drugs, antiviral therapy, drinking plenty of fluids, a balanced diet and proper nutrition3,5.
Up to contents
Possible complications
The prognosis for the disease is usually favorable. However, incorrect or untimely treatment can lead to the development of complications:
- The addition of a secondary bacterial infection, accompanied by a worsening of the sick child’s condition.
- Sometimes severe necrotizing forms of stomatitis lead to osteomyelitis - destruction of the bone tissue of the jaw.
- Persistent or frequent stomatitis can provoke the loss of teeth from both the primary and permanent sets.
- The presence of a chronic purulent inflammatory focus in a child’s body negatively affects the state of immunity, and also, under the influence of unfavorable factors, can lead to blood poisoning - sepsis.
Recommendations during treatment
It is very important to provide proper hygienic care for the baby during treatment. All toys must be thoroughly washed with hot water and baby or laundry soap. Wet cleaning should be carried out daily. It is best to wash the floors in the children's room with plain water, without adding disinfectants, as they often cause allergic reactions. It is necessary to ventilate the room in which the child spends most of his time at least 6 times a day. The last airing should be done before bedtime and last at least 30 minutes.
Children's dishes and bottles, as well as pacifiers and pacifiers, must be sterilized. To care for the skin, the baby must have his own towel - you cannot use towels used by other family members for this purpose, because the bacterial flora of an adult and an infant is very different.
Remedies for stomatitis in children
To speed up the healing of ulcers and the child’s recovery, you need to:
- keep plenty of fluids (breastfed children should be given breastfeeding “on demand”);
- if the child receives complementary feeding, make sure that all food is in liquid or puree form (the introduction of crackers and baby cookies into the diet should be postponed until complete recovery);
- increase the duration of daytime sleep - this will allow you to quickly restore strength and avoid overexertion, which is contraindicated for sick babies.
Feeding the baby
If, despite all the measures taken, the child’s condition does not improve after three days of treatment, it is necessary to visit the doctor again to rule out other diseases. After recovery, a preventive regimen and measures aimed at strengthening the immune system should be provided: hardening, gymnastics, frequent walks, water treatments. They must correspond to the age and physiological characteristics of the child, so before starting any health procedures it is better to consult a specialist.
Prevention in infants
Preventive measures should begin in a newborn child immediately after he is discharged from the maternity hospital. For the first days and months of life, it is necessary to adhere to thorough disinfection of toys, bottles during artificial feeding, or to treat the nipples immediately before applying to the breast.
«
An important point is regular visits to the dentist from the first teeth. It is necessary to carefully care for your baby’s oral cavity and use only special toothbrushes and toothpastes, preferably those recommended by the doctor.
Angular stomatitis in a child
Causes
In children, seizures are most often a manifestation of allergies, and can also appear while taking antibiotics. The mechanism is as follows: when using antibiotics, the microflora of the oral cavity is disrupted (both harmful and beneficial microbes die), against this background, space is freed up in which Candida fungi settle. It is these fungi that eventually cause the formation of buttocks.
Similar erosions can appear against the background of herpetic lesions, injuries, allergies, dry lips and cracks. It is important to determine the cause of their appearance and only then prescribe treatment.
Symptoms
Angular stomatitis (jams) - erosions with crusts that appear in the corners of the mouth - is also a fairly common form of stomatitis.
Treatment
- Antiseptics (chlorhexidine, miramistin) - use a gauze swab or ear stick to treat the surface of the wound.
- Keratoplasty (solcoseryl, oil solution of vitamins A and E) - applied to a dry surface after antiseptic treatment.
- Fighting the cause of the disease (if it is an allergy, we remove the allergens and prescribe antihistamines, if it is due to antibiotics, we prescribe drugs to restore the microflora and antifungal ointments, etc.).
What is stomatitis
Stomatitis is an inflammatory process on the oral mucosa
In the medical literature, stomatitis is an inflammatory disease of the oral mucosa, characterized by the appearance of small white ulcers on the inner surface of the lips, gums, tongue and throat.
Depending on the cause, it may be aphthous or infectious stomatitis. The pathology is manifested by pain, general malaise and other symptoms.
The mucous membrane of epithelial origin covers almost the entire surface of the oral cavity. Special cells of the mucous membrane not only protect internal tissues, but also secrete various substances. Also in the oral cavity there are salivary glands necessary to ensure primary digestive functions.
When an ulcer occurs, the mucous membrane is damaged and the function of the surface epithelium is disrupted. As a rule, the disease has a benign course, but in rare cases dangerous complications may develop.
Small ulcers with stomatitis may appear during the day. Even without treatment, the inflammatory process is self-limiting within 7-10 days. However, large ulcers often require long-term treatment.
Stomatitis can also become chronic. In this case, foci of inflammation will appear periodically in different parts of the oral mucosa. Untimely or incorrect treatment contributes to relapses.
Types of pathology
Temperature with stomatitis in children
Stomatitis is classified according to the form of its course, source of occurrence and characteristic features. Main types:
- Aphthous stomatitis is the appearance of ulcers of an inflammatory nature. This is the most common form of pathology among children. Signs include the appearance of sores that are pale white or yellowish in color with a red outer ring in the mouth. This may be one formation or several ulcers at once in different areas. Typical places of occurrence are the tissues of the inner lips and cheeks. Painful sensations are usually not expressed. In addition, the aphthous form is not contagious.
- Herpetic stomatitis is an infectious pathology of the oral cavity that develops due to invasion of the herpes virus. The disease is characterized by the appearance of small, painful, fluid-filled ulcers in the mouth. Foci of infection may appear on the outer surface of the lips. A yellow crust usually forms around the ulcer. Within 5-7 days, the source of infection disappears, however, the herpetic form of the disease is characterized by a relapsing course.
- Candidal stomatitis is an infectious lesion of the oral cavity as a result of invasion of the Candida fungus. This form is usually diagnosed in children and elderly patients. Chronic course is also characteristic.
- Allergic stomatitis is a lesion of the oral mucosa as a result of sensitization of the immune system. Additional symptoms include facial redness, neck swelling, and itching.
- Aphthous stomatitis is the most benign form. This pathology occurs rarely and goes away on its own without the risk of developing a chronic form of the course. Fungal and viral forms of stomatitis, on the contrary, are quite dangerous.