Causes of glossitis
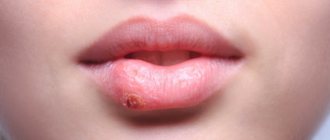
Glossitis can be an independent disease caused by bacteria, or a sign of a certain systemic pathology. Microtraumas and viruses usually lead to local damage to the tongue. For example, herpes very often not only affects the mucous membrane of the oral cavity, but also causes the occurrence of stomatitis and glossitis.
Inflammation of the tissues of the tongue can be a consequence of a burn to the mouth or frequent consumption of too hot drinks. Open gates for infection that causes glossitis are mechanical injuries to the oral cavity and tongue. Provoking factors also include:
- smoking, alcohol abuse;
- eating spicy foods;
- using a mouth freshener;
- frequent use of mouth rinses;
- poisoning with salts of heavy metals;
- injury to the tongue by destroyed sharp teeth;
- frequent exposure of the skin of the tongue to chemical irritants and electric current.
Causes of chronic glossitis:
- decreased immunity;
- dysbacteriosis;
- conditions that cause autoantibodies to be produced.
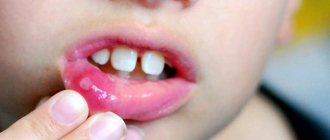
Causes of glossitis in children
Glossitis occurs in children for various reasons. Most often it is provoked by the child constantly biting his tongue. An incorrectly selected brace system can also lead to problems. Desquamative glossitis in young patients is a consequence of helminthic infestations, atopic dermatitis, and blood diseases. In this case, there are usually no difficulties when chewing and swallowing food.
Candidal glossitis in children develops against the background of diabetes mellitus and long-term use of antibiotics.
Phlegmonous
Since phlegmonous glossitis affects not only the entire thickness of the tongue, but also spreads further, to the lower part of the oral cavity and even the chin and neck, it is considered to be deep glossitis. The main symptom of this disease is the formation of phlegmons and abscesses, accompanied by a sharp deterioration in the patient’s general condition with fever, severe headaches, swelling and soreness of the tongue, and difficulty breathing. Treatment of deep glossitis must begin at the first signs of its appearance. Purulent formations are removed surgically, followed by the administration of antibacterial drugs.
Symptoms of glossitis
Glossitis is manifested by the following general symptoms:
- sensation of a foreign body in the mouth;
- burning tongue;
- discoloration of the skin of the tongue to bright red or burgundy;
- swelling of the tongue;
- increased salivation;
- dullness or complete loss of taste sensations (perversion of taste is possible);
- difficulty in swallowing;
- slurred speech, severe pain during conversation.
If treatment for glossitis is not carried out or is illiterate, the disease becomes chronic. Then dense, persistent swelling of the tongue occurs and its structure changes. In advanced forms, growths may form. The onset of an abscess is indicated by an uneven increase in size of the organ. Then the pain syndrome becomes pronounced.
If glossitis is complicated by phlegmon, purulent discharge appears on the surface of the tongue, and the process of chewing and swallowing food is disrupted. Attacks of suffocation may occur and speech becomes difficult. The body temperature rises, the lymph nodes become enlarged, and weakness increases.
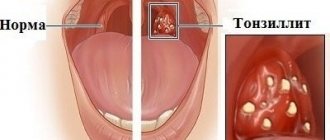
Signs of glossitis caused by bacterial and viral microflora
Glossitis of the tongue, which is caused by pathogenic microflora, manifests itself with symptoms:
- local increase in temperature;
- soreness;
- edema;
- hyperemia.
If the disease is provoked by viruses, it may be characterized by vesicles, after opening which small erosions remain on the mucous membrane. In this case, the taste organ becomes too dense or, conversely, excessively loose, and hyperplastic changes are observed.
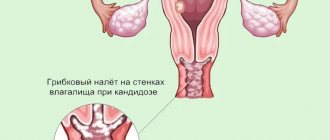
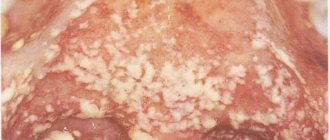
Candidal glossitis looks in the photo as a white coating on the tongue.
Symptoms of different types of glossitis
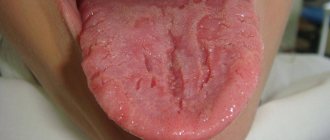
Desquamative glossitis, which is also called “geographical tongue,” usually develops against the background of gastrointestinal diseases. When examining a patient, the doctor sees a tongue cut with grooves and lines, which may resemble the outlines of the continents. The formation of the disease is promoted by:
- blood diseases;
- metabolic disorders;
- parasites.
Bright red spots with desquamative glossitis are located on the front surface and sides of the tongue. In this case, the patient complains of moderate pain and burning.
Deep glossitis is always localized at the “bottom” of the oral cavity. Inflammation can spread to the neck and chin area. Untimely treatment of this type of pathology leads to an abscess.
Diamond-shaped or median glossitis is manifested by thickening of the epithelium and the formation of diamond-shaped areas in the basal region of the tongue. Their color can be bright red or bluish. The form is prone to chronicity and relapse. Very rarely, rhomboid glossitis can be characterized by other signs. Thus, the diamond-shaped areas may become smooth and atrophy (flat form) or dense, bumpy growths may form on the surface of the tongue (warty form of rhomboid glossitis).
Folded glossitis is a congenital anomaly. These are folds on the back of the tongue. The deepest of them runs longitudinally along the midline of the taste organ. Since the disease does not cause discomfort, no special treatment is carried out (only for aesthetic purposes).
The main symptom of villous glossitis is the proliferation of filiform papillae, which subsequently become keratinized and look like small villi. The problem most often occurs with constant trauma to the tongue or with candidiasis.
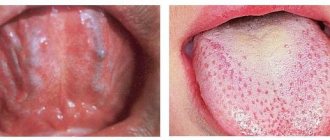
Gunter's glossitis indicates the development of folate deficiency or B12 deficiency anemia. The tongue becomes very smooth and acquires a bright crimson color. Taste buds atrophy.
Interstitial glossitis (precancerous form) may indicate infection with syphilis. Part of the muscle tissue is replaced by connective tissue. The tongue looks like a quilt. Some of its parts are elevated, the grooves of connective tissue strongly tighten the edges. If treatment is not started, the muscle tissue completely degenerates into connective tissue.
If you notice similar symptoms, consult a doctor immediately. It is easier to prevent a disease than to deal with the consequences.
Treatment
Depending on the causes and situation, treatment of desquamative glossitis may involve a combination of different methods:
- the use of local preparations (rinses) to relieve itching and discomfort;
- elimination of underlying diseases that affect the appearance of such a symptom;
- a gentle diet that does not irritate the tongue while eating;
- use of anti-inflammatory, vitamin-mineral, antihistamines, sedatives and other drugs - as prescribed by a doctor;
- novocaine blockades if the pain is severe and complicates the patient’s life;
- physiotherapy: ultraphonophoresis, ultrasound therapy, etc.
During the treatment process, it is important not to miss the underlying disease, which affects the appearance of signs of desquamative glossitis (if any). Otherwise, the patient will return to unwanted symptoms again and again until the main disease is discovered.
Diagnosis of glossitis
Pronounced symptoms allow dentists and therapists (it is these doctors who treat glossitis) to judge the presence of one form or another of the disease. To assess the depth and nature of the lesion, as well as to diagnose the disease that provoked the development of glossitis, different methods are used:
- bacteriological;
- cytological;
- biochemical;
- histological;
- serological.
All these diagnostic methods are available in any modern dental clinic
. To exclude the presence of syphilis, microscopy of the scraping is performed for Treponema pallidum, and an anticardiolipin test (allows us to detect antibodies to the cardiolipin antigen present in the blood of patients with syphilis). If it is necessary to determine the causative agent of glossitis, the following is carried out:
- PCR diagnostics (detection of the pathogen by its DNA);
- Enzyme-linked immunosorbent assay (ELISA). For analysis, blood is taken from a vein. The study is aimed at identifying specific antibodies produced by the patient’s body against the pathogen.
Candida
The name comes from the pathogens, fungi of the genus Candida, which provoke this disease, so another common name is fungal glossitis. In addition, it is often called yeast glossitis. This disease indicates the presence of a fungal infection in the body and a sharp decrease in the level of immunity. Chronic candidal glossitis is characterized by exacerbations when the body's immune response is weakened due to seasonal respiratory and other infectious diseases. Most often, this disease affects newborn children and people after long-term antibiotic therapy. Yeast is treated with antifungal drugs, as well as immunomodulators.
How and with what to treat glossitis of the tongue in adults and children
Treatment of tongue glossitis requires elimination of the diseases that led to its appearance. This refers to anemia, gastrointestinal diseases, syphilis, etc. To minimize pain, you need to rinse your mouth with Furacilin, a solution of Chlorhexidine (0.05%) or potassium permanganate, and avoid eating rough food. In case of severe pain, local applications with anesthetics can be made:
- Trimecaine solution (2%);
- Lidocaine solution;
- Pyromecaine solution.
If the tongue is dry, it should be lubricated with a mixture of glycerin and Anestezin.
For a speedy recovery, the skin of the tongue must be cleaned of plaque using a cotton swab soaked in proteolytic enzymes (Chymotrypsin, Trypsin). If there are painful ulcers, these drugs for the treatment of tongue glossitis can be replaced with applications with Iruksol. After the hygiene procedure, it is important to treat the cleaned lesions with antiseptics. This helps prevent secondary infection and also prevents the development of serious complications.
To speed up regeneration processes, gel and jelly-like medicines with solcoseryl, as well as preparations containing vitamin A, can be used. The mixture formed by rosehip oil and vitamin A heals the affected skin well and relieves pain.
If excessive thickening of the stratum corneum of the epidermis (hyperkeratosis) is observed, surgical intervention is ordered. Antifungal, antibacterial and anti-inflammatory drugs are selected taking into account the severity of the disease and the dominant symptoms.
All patients with glossitis can take immunomodulators. Hormones are used extremely rarely - only for difficulty breathing. To avoid atrophy of taste organ cells, Hydrocortisone and Prednisolone ointments are prescribed in short courses.
How to treat tongue glossitis at home
Treatment of tongue glossitis at home can be carried out using traditional medicine recipes:
- decoction of chamomile flowers. 1 tbsp. pour a glass of boiling water over the flowers. Infuse, strain. Rinse your mouth after every meal;
- bedstraw decoction. 1 tbsp. pour a glass of boiling water. Leave for 30 minutes. Take 50 ml orally after meals and rinse the mouth 3-4 times a day. Similarly, you can use decoctions of sage and basil;
- soda solution. Add 2-3 drops of iodine and a teaspoon of baking soda to a glass of warm water. Rinse your mouth 3 times a day;
- natural honey Slowly dissolve a spoonful of honey;
- propolis. Lubricate the areas of inflammation 5 times a day. Instead of propolis, you can use raw carrot/potato juice or rosehip oil;
- tea tree oil. Dilute in equal proportions with olive, sunflower or sea buckthorn oil. Treat glossitis lesions 5 times a day or keep it in your mouth for several minutes.
How to avoid getting sick
Preventive measures include following simple rules:
- balanced diet;
- elimination of traumatic effects on the tissues of the tongue;
- taking an antifungal drug during a course of antibiotics and hormones;
- course use of immunomodulators;
- maintaining oral hygiene;
- timely treatment of emerging dental diseases.
People who take care of their dental health and visit the dentist twice a year are much less likely to experience tongue candidiasis. This is a proven fact. Therefore, do not ignore your doctor’s requests to come for preventive examinations.