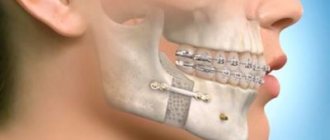
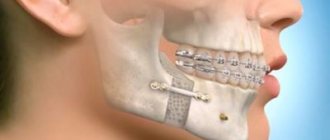
What is it and how to treat it?
Osteomyelitis is an inflammation of the bone marrow with a tendency to progress.
This is what distinguishes it from the widespread dentoalveolar abscess, dry socket, and osteitis seen in infected fractures. Osteomyelitis affects adjacent cortical plates and often periosteal tissues. In the era of preantibiotics, osteomyelitis of the mandible was not uncommon. With the advent of antibiotics, the disease began to be detected less frequently. But in recent years, antimicrobial drugs have become less effective, and the disease has reappeared.
Diagnostics
Identifying this complex disease requires professionalism and experience from the doctor: the difficulty of diagnosis is explained by fairly general symptoms that are easily confused with many other diseases.
After a conversation with the patient and a visual examination, a jaw photograph is necessarily taken, in which you can distinguish:
- unevenness of the bone structure (there are both areas with compaction of bone tissue and with its deficiency);
- blurred jaw contour due to the presence of pus;
- thickening of the top layer of bone.
With hematogenous osteomyelitis, X-rays clearly show signs of bone tissue destruction, and compactions collect at the base of the causative tooth.
In particularly dangerous and advanced cases, simple and specialized blood tests are prescribed to diagnose the disease, helping to determine the content of certain substances in it and possible deviations from the norm.
Sometimes, to complete the clinical picture, biochemical tests of purulent fluid are prescribed.
Osteomyelitis of the jaw. Causes
In the maxillofacial region, osteomyelitis occurs mainly as a result of the continuous spread of odontogenic infections or as a result of trauma. Primary hematogenous osteomyelitis in the maxillofacial region is rare, usually in very young people. Thus, osteomyelitis of the jaw occurs after tooth extraction, root canal treatment, or with fractures of the upper or lower jaw. This initial lesion leads to an inflammatory process caused by bacteria.
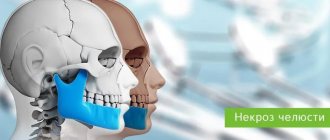
The incidence of osteomyelitis is much higher in the mandible due to the dense, poorly vascularized cortical plates and blood supply. Osteomyelitis of the maxilla is much less common due to the excellent blood supply from several feeding vessels. In addition, the maxillary bone is less dense than the mandibular bone.
Reduced patient protection, both local and systemic, may significantly contribute to the development of osteomyelitis. Osteomyelitis can be associated with a variety of systemic diseases, including diabetes, autoimmune conditions, malignancies, malnutrition, and acquired immunodeficiency syndrome. Medicines associated with the risk of osteomyelitis: steroids, chemotherapy drugs, bisphosphonates. Radiation therapy (causes so-called radiation osteomyelitis of the jaw), osteoporosis and bone pathology can change the blood supply to this area and become a potential springboard for the development of osteomyelitis.
Osteomyelitis
Manifestations of acute osteomyelitis depend on the route of infection, the general condition of the body, the extent of traumatic damage to the bone and surrounding soft tissues. On radiographs, changes are visible 2-3 weeks after the onset of the disease.
Hematogenous osteomyelitis
As a rule, it develops in childhood, with a third of patients becoming ill before the age of 1 year. Quite rare cases of the development of hematogenous osteomyelitis in adults are actually relapses of the disease suffered in childhood. Most often it affects the tibia and femur. Multiple bone lesions are possible.
From a remote source of inflammation (soft tissue abscess, phlegmon, infected wound), microbes are carried through the blood throughout the body. In long tubular bones, especially in their middle part, a wide network of vessels is well developed, in which the speed of blood flow slows down. Infectious agents settle in the cancellous bone. Under unfavorable conditions (hypothermia, decreased immunity), microbes begin to multiply rapidly, and hematogenous osteomyelitis develops. There are three forms of the disease:
Septic-pyemic form
. Characterized by an acute onset and severe intoxication. Body temperature rises to 39-40°, accompanied by chills, headache and repeated vomiting. Possible loss of consciousness, delirium, convulsions, hemolytic jaundice. The patient's face is pale, lips and mucous membranes are bluish, and the skin is dry. The pulse is increased, the pressure is reduced. The spleen and liver enlarge, and sometimes bronchopneumonia develops.
On the 1st-2nd day of the disease, precisely localized, sharp, drilling, bursting or tearing pain appears in the affected area, intensifying with the slightest movements. The soft tissues of the limb are swollen, the skin is hot, red, and tense. When it spreads to nearby joints, purulent arthritis develops.
After 1-2 weeks, a focus of fluctuation (fluid in the soft tissues) forms in the center of the lesion. Pus penetrates the muscles, intermuscular phlegmon is formed. If the phlegmon is not opened, it can open on its own with the formation of a fistula or progress, leading to the development of periarticular phlegmon, secondary purulent arthritis or sepsis.
Local form
. The general condition suffers less and sometimes remains satisfactory. Signs of local inflammation of bone and soft tissue predominate.
Adynamic (toxic) form
. Rarely seen. Characterized by lightning-fast onset. The symptoms of acute sepsis predominate: a sharp increase in temperature, severe toxicosis, convulsions, loss of consciousness, a pronounced decrease in blood pressure, acute cardiovascular failure. Signs of bone inflammation are weak and appear late, which makes diagnosis and treatment difficult.
Post-traumatic osteomyelitis
Occurs with open bone fractures. The development of the disease is facilitated by contamination of the wound at the time of injury. The risk of developing osteomyelitis increases with comminuted fractures, extensive soft tissue damage, severe concomitant injuries, vascular insufficiency, and decreased immunity.
Post-traumatic osteomyelitis affects all parts of the bone. In linear fractures, the area of inflammation is usually limited to the fracture site; in comminuted fractures, the purulent process tends to spread. Accompanied by hectic fever, severe intoxication (weakness, weakness, headache, etc.), anemia, leukocytosis, increased ESR. The tissues in the area of the fracture are swollen, hyperemic, and sharply painful. A large amount of pus is released from the wound.
MRI of the foot. Osteomyelitis of the talus and tibia with the presence of an extensive area of bone tissue destruction.
Gunshot osteomyelitis
More often occurs with extensive lesions of bones and soft tissues. The development of osteomyelitis is promoted by psychological stress, decreased body resistance and insufficient wound treatment.
General symptoms are similar to post-traumatic osteomyelitis. Local symptoms in acute gunshot osteomyelitis are often mild. The swelling of the limb is moderate, there is no profuse purulent discharge. The development of osteomyelitis is indicated by a change in the wound surface, which becomes dull and covered with a gray coating. Subsequently, inflammation spreads to all layers of the bone.
Despite the presence of a focus of infection, with gunshot osteomyelitis, bone fusion usually occurs (the exception is significant bone fragmentation, large displacement of fragments). In this case, purulent foci end up in the callus.
Postoperative osteomyelitis
It is a type of post-traumatic osteomyelitis. Occurs after osteosynthesis operations of closed fractures, orthopedic operations, insertion of wires when applying compression-distraction devices or applying skeletal traction (wire osteomyelitis). As a rule, the development of osteomyelitis is caused by non-compliance with asepsis rules or a highly traumatic operation.
Contact osteomyelitis
Occurs due to purulent processes in the soft tissue surrounding the bone. Especially often, the infection spreads from soft tissue to the bone with panaritium, abscesses and phlegmon of the hand, and extensive wounds of the scalp. Accompanied by increased swelling, increased pain in the area of injury and the formation of fistulas.
Treatment
Only in hospital in the traumatology department. The limb is immobilized. Massive antibiotic therapy is carried out taking into account the sensitivity of microorganisms. To reduce intoxication, replenish blood volume and improve local blood circulation, plasma, hemodez, and 10% albumin solution are transfused. For sepsis, methods of extracorporeal hemocorrection are used: hemosorption and lymphosorption.
A prerequisite for successful treatment of acute osteomyelitis is drainage of the purulent focus. In the early stages, burr holes are made in the bone, followed by washing with solutions of antibiotics and proteolytic enzymes. For purulent arthritis, repeated punctures of the joint are performed to remove pus and administer antibiotics; in some cases, arthrotomy is indicated. When the process spreads to soft tissues, the resulting ulcers are opened, followed by open rinsing.
Osteomyelitis of the jaw. Symptoms
Like any infection of the maxillofacial area, osteomyelitis of the lower jaw and osteomyelitis of the upper jaw are accompanied by symptoms:
- pain
- swelling and redness on the surface of the skin
- adenopathy
- heat
- paresthesia of the inferior alveolar nerve
- lockjaw
- malaise
- fistulas
Pain from osteomyelitis is often described as deep and aching, which often does not correspond to the clinical picture.
In acute osteomyelitis, swelling and erythema of the overlying tissues are very often observed, which indicate the initial phase of the inflammatory process in the underlying bone.
Fever often accompanies acute osteomyelitis, whereas it is relatively rare in chronic osteomyelitis.
Inferior alveolar nerve paresthesia is a classic sign of pressure on the inferior alveolar nerve as a result of an inflammatory process in the bone marrow of the mandible.
Trismus may be present due to an inflammatory reaction in the muscles of mastication.
The patient usually experiences malaise or a feeling of general weakness, which can accompany any systemic infection.
Finally, both intraoral and extraoral fistulas are usually present in the chronic phase of maxillofacial osteomyelitis.
OSTEOMYELITIS OF THE EXTREMITIES
- CLASSIFICATION
- NON-SPECIFIC OSTEOMYELITIS
- SPECIFIC OSTEOMYELITIS
- CAUSES
- PHOTO OF OSTEOMYELITIS
- TREATMENT OF OSTEOMYELITIS OF THE EXTREMITIES
- ACUTE HEMATOGENIC OSTEOMYELITIS
- POST-TRAUMATIC AND POST-OPERATIVE OSTEOMYELITIS
- OSTEOMYELITIS OF JOINTS AND SPINE
- HEMODIALYSIS AND DRUG ADDICTION
- SICKLE CELL ANEMIA
Content
Osteomyelitis is an inflammatory process of a purulent-necrotic nature that affects the bone tissue surrounding the periosteum and bone marrow. The causative agents of osteomyelitis, in the vast majority of cases, are staphylococci and streptococci.
Osteomyelitis that occurs for the first time is called acute. If the patient has a protracted course of the disease with exacerbations and remissions, then we are talking about a chronic course of the inflammatory process of osteomyelitis. Often, with osteomyelitis, the entire bone tissue, including the bone marrow area, is involved in the inflammation process. In the chronic process of osteomyelitis, bone sclerosis and deformation occur.
Osteomyelitis of the jaw. Diagnostics
Patients are often given laboratory tests as part of their initial evaluation. In the acute phase of osteomyelitis, leukocytosis with a shift to the left is often observed, which is typical for any acute infection. But leukocytosis is relatively rare in the chronic phases of osteomyelitis.
The patient may also have an elevated erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP). Both ESR and CRP are very sensitive. Almost all patients will undergo maxillofacial imaging.
Computed tomography (CT) has become the standard of care in the evaluation of maxillofacial pathology such as osteomyelitis. It provides a three-dimensional image. CT can provide very detailed images of early cortical bone erosion in osteomyelitis. Often, along with pathological fractures, you can see the degree of damage and bone sequestration. CT scanning, like conventional X-ray examination, shows changes when bone demineralization reaches 30 to 50%, which significantly delays the diagnosis of osteomyelitis. Magnetic resonance imaging (MRI) is generally considered more valuable in assessing soft tissue lesions in the maxillofacial region. However, MRI can help in the early diagnosis of osteomyelitis. Thus, MRI can help in identifying the early stages of osteomyelitis.
TREATMENT OF OSTEOMYELITIS OF THE EXTREMITIES
When treating osteomyelitis, mandatory hospitalization is indicated. Along with surgical treatment of the affected area, it is necessary to prescribe massive antibiotic therapy (intravenous and intramuscular administration of antibacterial drugs), powerful detoxification therapy (plasma transfusions and blood substitutes), immunostimulants, vitamin therapy, hemosorption, hyperbaric oxygenation.
ACUTE HEMATOGENIC OSTEOMYELITIS
When treating acute hematogenous osteomyelitis in children under six years of age, the following is indicated:
- Cefuroxime and Amoxicillin/Clavulanate (first-line drugs);
- Ampicillin/Sulbactam;
- Ceftriaxone and Oxacillin (alternative drugs);
For children over six years of age and adults, the following are used for the treatment of acute hematogenous osteomyelitis:
- Oxacillin and Gentamicin;
- Amoxicillin/Clavulanate (first-line drugs);
- Cefuroxime;
- Cephalozolin and Netilmicin;
- Lincomycin and Gentamicin;
- Clindamycin and Gentamicin;
- Fluoroquinolone and Rifampicin (alternative drugs);
POST-TRAUMATIC AND POST-OPERATIVE OSTEOMYELITIS
For post-traumatic and postoperative osteomyelitis, the following are prescribed:
- Ofloxacin;
- Ciprofloxacin and Lincomycin (first-line drugs);
- Cefepime;
- Vancomycin and third-fourth generation cephalosporins;
- Imipenem;
- Linezolid and Ceftriaxone;
OSTEOMYELITIS OF JOINTS AND SPINE
For osteomyelitis of the joints and spine the following are prescribed:
- Oxacillin;
- Ceftriaxone and Aminoglycosides (first-line drugs);
- Ciprofloxacin and Rifampicin (alternatives);
HEMODIALYSIS AND DRUG ADDICTION
For patients on hemodialysis and drug addicts, the following are used:
- Oxacillin and Ciprofloxacin;
- Vancomycin and Ciprofloxacin;
SICKLE CELL ANEMIA
For patients with sickle cell anemia:
- Ciprofloxacin or third generation cephalosporins (Ceftriaxone, Cefotaxime, Cefoperazone).
Osteomyelitis of the jaw. Treatment
The first step in treating osteomyelitis is to correctly diagnose the condition. A preliminary diagnosis is made based on clinical assessment and radiological examination.
Treatment of osteomyelitis of the maxillofacial region requires both conservative and surgical methods. In later stages, antibiotic therapy is rarely effective, so the vast majority of cases of osteomyelitis require surgery.
For osteomyelitis of the upper or osteomyelitis of the lower jaw, as a rule, classical treatment is used - sequestrectomy. The goal is to remove necrotic or poorly vascularized bone sequestration in the infected area and improve blood flow. Sequestrectomy involves removing infected and avascular pieces of bone—usually cortical plates—in the infected area. Visual assessment is critical at these stages, but radiation diagnostics, which shows the osseous extent of the pathology, also helps. It is often necessary to remove teeth adjacent to the area of necrosis.
Supporting the weakened area with a fixation device (external fixator or reconstruction plate) is often used to prevent pathological fracture.
Treatment
The effectiveness of therapy depends on the initial causes of the formation of the inflammatory process. Therefore, in osteomyelitis of the jaw, comprehensive treatment is important, not only by a dentist, but it is recommended to go for a consultation with doctors of medical specialties.
- Sanitation of the oral cavity with antiseptic solutions. Further spread of infection to surrounding structures is prevented. Also, necrotic soft tissue formations are eliminated.
- Anti-inflammatory drugs. Minimize intoxication of the body.
- Immobilize the fracture, and if there is a tooth in it, then remove it.
- Taking antibiotics, regardless of provoking factors.
- Intraosseous lavage may be necessary and will provide positive results. Minimizes the occurrence of complications and quickly prevents the growth of a harmful process.
- In case of a fistula, sequestrectomy is performed - necrotic areas of bone tissue are eliminated under anesthesia, taking into account the extent of the damage.
- If the teeth are mobile, they are splinted.
- After eliminating symptoms and carrying out all interventions, physical therapy, vitamins and immunomodulators are recommended.
Prevention of such pathology consists only of timely and regular visits to the dentist’s office and treatment of pathological processes in the oral cavity. Do not treat yourself at home, so as not to make it worse. Also, it is necessary to strengthen the body’s immune system, avoid injuries and not let the pathological process become chronic.